|
4/18/2024 0 Comments Child cervical spine x ray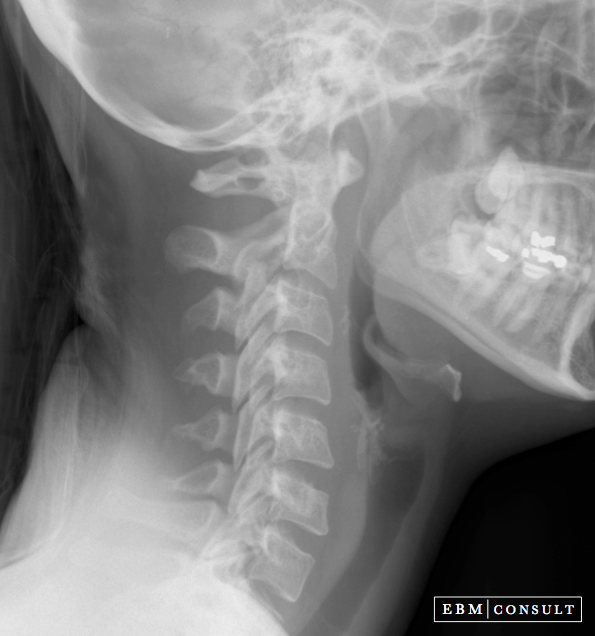
In a subset analysis, the NEXUS criteria had a 100% sensitivity and a 19.9% specificity for detecting clinically significant CSI in pediatric victims of blunt trauma. 7 On the other hand, the NEXUS study included 3,065 patients under the age of 18. Unfortunately, the Canadian C-spine study excluded all patients younger than age 16 and has not been validated in the pediatric population. 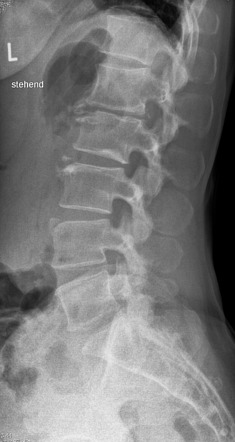
6 Decision RulesĬlinical decision rules such as the NEXUS criteria and the Canadian C-spine Rule are frequently utilized in adult trauma. Juvenile rheumatoid arthritis and osteogenesis imperfecta, as well as other rare predisposing medical conditions - Klippel-Feil syndrome, Larsen syndrome, and Morquio syndrome - should also raise one's suspicion for CSI in the appropriate clinical setting. Isolated congenital vertebral anomalies such as os odontoideum (separation of the odontoid process from the body C2) can cause serious CSI from even minor trauma. Specifically, children with Down syndrome are at increased risk for C1/C2 subluxation due to their relative atlantoaxial instability and articular mobility. Patient, it is also important to consider any other congenital or acquired comorbidity that may predispose them to CSI. Older children and adolescents are additionally at risk for sports-related CSI, diving incidents, and accidents involving other forms of motorized transportation. The most common causes of pediatric CSI include motor vehicle collisions (MVCs), falls, pedestrian accidents, and bicycle collisions, with MVCs spanning all ages but much more commonly causing significant CSI in young pediatric patients. Not surprisingly, 60-80% of all pediatric spine injuries occur in the C-spine, compared to adults, in whom CSIs comprise only 30-40% of all spine injuries. These characteristics place young children at a dangerously increased risk for higher level CSI and ligamentous disruption. 3 In addition, their paraspinal musculature is underdeveloped, ossification centers have not yet formed, and interspinous ligaments have greater laxity. 2 Young children in particular have larger and heavier craniums relative to their body size, resulting in a higher center of gravity and fulcrum for cervical motion (C2-C3 versus C5-C6 in adolescents and adults). The pediatric C-spine remains underdeveloped until at least 8 years of age, at which time it begins taking on characteristics of an adult C-spine. 
1 As an emergency physician, you must be proficient in evaluating pediatric patients for traumatic CSI. While cervical spine injuries (CSIs) are relatively rare in this patient population (<1%), they can be associated with significant morbidity and mortality. You find it difficult to discern if he has any midline cervical spine tenderness and begin to wonder: Does this patient need cervical spine imaging? If so, what type of imaging should be obtained? Can I apply the same clinical decision rules that I use in my adult patients?Īge-related anatomic differences and injury patterns, as well as difficulties with the physical exam, make clearing the cervical spine (C-spine) one of the most challenging aspects of pediatric trauma care. He has a cervical collar in place and is crying hysterically. GCS is 15, and he has no other obvious distracting injuries. On your initial examination, vital signs are significant only for tachycardia. He was the restrained backseat passenger of a vehicle that was rear-ended at 50 mph while stopped in traffic. A 4-year-old boy is brought to the emergency department after a high-speed motor vehicle collision.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
